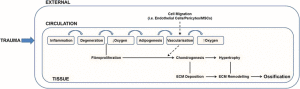
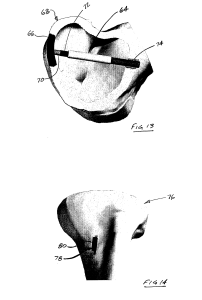
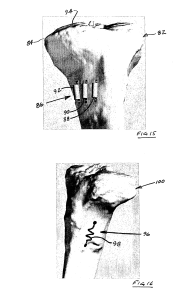
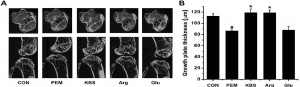
How does bone know how to be the proper shape and size for development? Can we manipulate this to grow taller?
I received this email from the author regarding how distraction osteogenesis would affect how bone manipulates growth in regards to maintaining placement of superstructures:
“It is indeed an interesting question as it challenges the system with an unnatural manipulation – i.e. interstitial growth.
The simple answer is: we haven’t tried, so I can’t say for sure.
If the relative locations of ligament and tendon insertions are what you are interested in, then previous works show that the periosteum is involved in regulation of their positions (see list below). Moreover, if the balance between proximal and distal growth rates is what you are interested in, then other works show that cross-sectional cutting and stripping of the periosteum can cause temporal acceleration in overall growth rate of the bone (also in humans, if I remember correctly), followed by a potential change in proximal to distal growth balance (I don’t think that these works test how these influence the positioning of superstructures in the bone; see list below).
Therefore, if the operation you are applying includes anchoring of the periosteum to the bone or its cutting and stripping, this is something that may influence the scaling of the bones.”
Isometric Scaling in Developing Long Bones Is Achieved by an Optimal Epiphyseal Growth Balance.
“One of the major challenges that developing organs face is scaling, that is, the adjustment of physical proportions during the massive increase in size. Although organ scaling is fundamental for development and function, little is known about the mechanisms that regulate it. Bone superstructures are projections that typically serve for tendon and ligament insertion or articulation and, therefore, their position along the bone is crucial for musculoskeletal functionality. As bones are rigid structures that elongate only from their ends, it is unclear how superstructure positions are regulated during growth to end up in the right locations. Here, we document the process of longitudinal scaling in developing mouse long bones and uncover the mechanism that regulates it. To that end, we performed a computational analysis of hundreds of three-dimensional micro-CT images, using a newly developed method for recovering the morphogenetic sequence of developing bones. the relative position of all superstructures along the bone is highly preserved during more than a 5-fold increase in length, indicating isometric scaling. It has been suggested that during development, bone superstructures are continuously reconstructed and relocated along the shaft, a process known as drift. most superstructures did not drift at all. Instead, we identified a novel mechanism for bone scaling, whereby each bone exhibits a specific and unique balance between proximal and distal growth rates, which accurately maintains the relative position of its superstructures. Moreover, we show mathematically that this mechanism minimizes the cumulative drift of all superstructures, thereby optimizing the scaling process. [There’s] a general mechanism for the scaling of developing bones. More broadly, these findings suggest an evolutionary mechanism that facilitates variability in bone morphology by controlling the activity of individual epiphyseal plates.”
If we can trick the bone into thinking it’s drifting maybe we can convince it to grow to maintain the position of the superstructure. For example, dislocating the bone or similar means.
Although the molecular mechanisms regulating each growth plate for different bones are similar the bones still have different elongation rates.
“superstructures, known as bone ridges, tuberosities, condyles, etc., are necessary for the attachment of tendons and ligament as well as for articulation. To perform these functions they are located at specific positions along the bone. Bone superstructures emerge during early skeletogenesis . During growth, bones elongate extensively by advancement of the two growth plates away from the superstructures. It is therefore expected that during elongation, superstructures would remain at their original position near the center of the bone. Nevertheless, the end result is proper spreading of superstructures along the mature bone, which clearly implies the existence of a morphogenetic mechanism that corrects their locations.”
It’d be interesting to see what happens to bone superstructures during distraction osteogenesis.
“An ossified bone is a rigid object and so are the superstructures protruding from it, implying that they cannot be relocated by means of cell migration or proliferation. Therefore, any scaling mechanism must be adapted to overcome these physical restrictions.”<-So we have to make the bone less rigid.
“forelimb bones tend to grow away from the elbow joint, whereas bones in hind limbs tend to grow toward the knee joint.”
” Because the periosteal sheath is stretched over the entire external surface of the bone, including both the superstructures and the growth plates, it can pass to the growth plates signals concerning the relative position of superstructures.”<-Then perhaps we can manipulate longitudinal bone growth by manipulating the periosteal sheath.
“periosteal tension down-regulates growth plate activity, as the higher the tension level, the more inhibited growth plate activity is. Damaged periosteum forms a scar tissue at the site of destruction. This scar tissue, which anchors the periosteum into the bone, creates an independent tension level near each growth plate. As a result, a new growth balance is formed, which equals the ratio between the distances from the site of the scar to the two ends of the bone, therefore maintaining the relative position of the scar site.. Superstructures can be considered as natural anchoring points for the periosteum into the ossified bone, either due to the insertion of tendons through them into the bone cortex, or by means of steric interference, such as in the tibiofibular junction. This results in a regulatory loop whereby the superstructures determine the tension levels of the two periosteal segments, which control the ratio of growth rates by inhibiting growth plate activity, which in turn maintains the relative position of the superstructure.”
Mechanical regulation of musculoskeletal system development
“During embryogenesis, the musculoskeletal system develops while containing within itself a force generator in the form of the musculature. This generator becomes functional relatively early in development, exerting an increasing mechanical load on neighboring tissues as development proceeds. A growing body of evidence indicates that such mechanical forces can be translated into signals that combine with the genetic program of organogenesis. This unique situation presents both a major challenge and an opportunity to the other tissues of the musculoskeletal system, namely bones, joints, tendons, ligaments and the tissues connecting them. Here, we summarize the involvement of muscle-induced mechanical forces in the development of various vertebrate musculoskeletal components and their integration into one functional unit.”
“These forces [on the cell cytoskeleton], which can be translated into biochemical signals by molecules possessing mechanotransduction capabilities, are transmitted across transmembrane receptors into the extracellular matrix (ECM) and can also reach neighboring cells.”
“In the case of musculoskeletal development, exogenous forces acting on tendons and the skeleton are generated by muscle contraction.”
“Bone morphology is regulated by mechanical forces at different levels, as demonstrated by the various developmental and functional aberrations that arise in the absence of muscle contraction. (1) Bone elongation is impaired due to reduced chondrocyte proliferation in the growth plate. (2) Additionally, the organization of resting chondrocytes into columns is impaired, which can also affect skeletal elongation. (3) Bone eminence growth is arrested, resulting in smaller or absent eminences. (4) Differential appositional growth is lost, resulting in a circular circumferential shape. (5) Joint formation is impaired during embryonic development, leading to joint fusion.”
“These effects on chondrocyte proliferation could be mediated by yes-associated protein 1 (YAP1), a mechanosensor that is part of the Hippo signaling pathway. Indeed, changes in YAP cellular localization in chondrocytes were identified in vitro in response to matrix stiffness, and YAP was shown to regulate bone size, promote chondrocyte proliferation and inhibit chondrocyte differentiation in vitro and in vivo by suppressing collagen type X”
“mechanical forces can regulate both the content and the dynamics of proteoglycan and collagen production by these cells”
“Bones grow in width by preferential periosteal growth, which involves repetitive steps of strut-and-ring construction by mineral deposition.”
“non-selective mechanosensitive cationic channels, PIEZO1 and PIEZO2, which are expressed in a variety of tissue types, including chondrocytes”
“the attachment between the very elastic tendon and the very rigid bone creates a point of high stress concentration during force transfer, which could lead to detachment. Dissipation of this stress is achieved either by the formation of fibrous attachments, in which tendon fibers are inserted into the cortical bone in a structure that resembles a root system, or by the formation of a fibrocartilaginous attachment composed of different layers that gradually change in stiffness. Although enthesis development begins in the embryo, the formation of the unique transitional tissue and its subsequent mineralization occur postnatally.”

Growth and mechanobiology of the tendon-bone enthesis
“In the mature skeleton, the tendon-bone enthesis is an interfacial zone of transitional tissue located between compliant, fibrous tendon to rigid, dense mineralized bone. This transitional tissue provides a mechanism of stress and strain reduction at the interface between two mechanically dissimilar tissues”
“Fibrous entheses are generally found at insertion sites of stabilizing tendons, whereas fibrocartilaginous entheses are typically found at insertions of tendons that contribute to joint movement. Fibrous enthesis attach directly to bone and typically form Sharpey’s fibers, which are perforating fibers that embed into bone’s periosteal surface”
“Fibrocartilaginous entheses consist of four distinct histological zones, including aligned tendon, unmineralized fibrocartilage, mineralized fibrocartilage, and subchondral bone. A smooth and uniform basophilic tidemark distinguishes the transition between the two fibrocartilaginous zones, and this tidemark is disrupted and irregular in enthesopathy. The fibrocartilage enthesis matures during postnatal growth in response to mechanical loads from skeletal muscle and consists of cells that express both tenogenic and chondrogenic factors”
“Morphologically, the development of the enthesis has been likened to a “miniature” or arrested growth plate. However, unlike growth plates in long bones which eventually fuse at skeletal maturity, the fibrocartilage of the enthesis retains the morphological features of fibrocartilage and maintain Gli1+ cells at the interface throughout postnatal growth”
Lasting organ-level bone mechanoadaptation is unrelated to local strain
“Bones adapt to mechanical forces according to strict principles predicting straight shape. Most bones are, however, paradoxically curved. To solve this paradox, we used computed tomography–based, four-dimensional imaging methods and computational analysis to monitor acute and chronic whole-bone shape adaptation and remodeling in vivo. We first confirmed that some acute load-induced structural changes are reversible, adhere to the linear strain magnitude regulation of remodeling activities, and are restricted to bone regions in which marked antiresorptive actions are evident.{this is actually a good finding because it emphasizes that bone is an adaptive tissue} We make the novel observation that loading exerts significant lasting modifications in tibial shape and mass across extensive bone regions, underpinned by (re)modeling independent of local strain magnitude, occurring at sites where the initial response to load is principally osteogenic. This is the first report to demonstrate that bone loading stimulates nonlinear remodeling responses to strain that culminate in greater curvature adjusted for load predictability without sacrificing strength.”
“Wolff’s law is at odds with the curved overall shape of most bones, however, because adherence to these principles would predict straighter bones.”
“bones is instead optimized for load predictability. This would lead to the prediction that as bone curvature increases and predictability of the bending direction is augmented, its strength decreases”
“bone acts as an organ to acquire lasting modifications in shape and strength with greater bending predictability, which involves coordination of spatial remodeling that is unrelated to local strain magnitude.”<-it could be unrelated to local strain magnitude because of fluid forces.
“acute bone gains are lost within 6 weeks after load and extend this by showing that this is achieved through a simple reversal, involving greater resorption and lower formation in the proximal tibia in the chronic phase”
“net load-induced acute gains in the mid-to-distal tibia are, in contrast, lasting. Our 4D analyses reveal that this gain in bone mass is achieved predominantly by an enhanced formation in the acute phase, with only minor subsequent modifications in remodeling in the chronic postload phase. Comparing the remodeling activities in these two diverse, proximal and distal, locations by our novel application of whole-bone 4D analyses leads us to propose that the rapidity of load-induced acute changes in bone remodeling and the rate of their chronic postload reversal are linked. Reversibility in the proximal tibia is aligned to a marked load-related antiresorptive effect, while, contrarily, the lasting adaptation in the mid-to-distal region is principally linked with load-induced osteogenesis. It is intriguing that only the latter leads to permanent modification in bone shape.”
“Long-term curvature changes in nonbiological materials can involve creep deformation.”
“We show that some acute load-induced structural changes are reversible and adhere to linear strain magnitude feedback-loop regulation of remodeling activities. On the other hand, a vast proportion of the bone retains lasting structural memory of loading to generate nonlinear, strain magnitude–independent remodeling to achieve greater curvature optimized for load predictability without sacrificing strength.”<-some bone changes may be due to creep deformation thus being permanent.