Getting a pump in your muscles may be a way to induce hydrostatic pressure but it is unlikely as lots of bodybuilders work towards achieving the pump so it’s something that occurs very frequently physiologically. So if the muscular pump did affect height it would likely be a phenomenon that would be noticed by now. But the goal of the pump is get the blood to the muscle under target not the bone. The pump is very localized to the muscle under tension so this may be why the muscular pump does not increase height. The target area for a hydrostatic pressure increase is the bone and the pump targets the muscle. This does not mean that an understanding of a muscular pump could help us understand how to increase hydrostatic pressure in the bone.
“A model is presented for enhancement of fluid flow through bone matrix and any porous tissue engineering scaffold implanted within it. The mechanism of enhancement is the skeletal muscle pump in compartments adjacent to the bone. Pressure waves from muscle pump contractions aided by increased blood pressure during exercise coupled with temporary occlusion of arteries leading to and veins from the bone, increase hydraulic pressure in cortical bone capillaries so as to amplify capillary filtration. It is proposed that capillary filtration increase is sufficiently convective to contribute to bone fluid flow and associated percolation through tissue engineered scaffold matrix implants. Importance of this contribution is its relative role in maintaining seeded cells in bioreactor scaffolds. Validation of the hypothesis starts at a minimum level of demonstrating that capillary filtration is convective. At a maximum level confirmation of the hypothesis requires demonstration that capillary filtration-based interstitial flow is sufficient to stimulate not only host bone cells (as proposed in part I of the hypothesis) but bioreactor-seeded cells as well. Preliminary data is presented supporting the prediction that skeletal muscle contraction generates convective capillary filtration.”
Although we don’t really want increased hydrostatic pressure in the capillaries that’s more likely to just deliver more nutrients to the bone. Increased hydrostatic pressure in capillaries increases capillary filtration getting more nutrients to the interstitial fluid. What we want is increased hydrostatic pressure in the interstitial fluid itself to encourage chondrogenic differenetiation.
“Nutrient exchange is not the sole function of transport in bone. There is increasing evidence that interstitial fluid flow is sensed by and modulates the behavior of bone cells. Percolation through bone matrix and associated implants is referred to as bone interstitial fluid flow
(BIFF). Two mechanisms for bone cell sensing of BIFF have been proposed; one mechanical and the other electrokinetic. The electrokinetic model focuses on streaming potentials that are putatively sensed by electrokinetic receptors in bone cell membranes. The mechanical model focuses on shear stress at the membrane-fluid interface, which is transmitted to second messenger by mechano-receptors”
“osteocytes and their processes are surrounded by relatively thin fluid (not necessarily Newtonian) annuli in the lacunar and canalicular compartments, rather than relatively large volumes of flowing blood.”
“muscle pump and exercise effects combine to increase capillary filtration sufficiently to add a significant component to BIFF. We reason that skeletal muscle, acting through a muscle pump mechanism, increases the rate of capillary filtration by increasing capillary hydraulic pressure via contraction of skeletal muscle in compartments adjacent to bone. Exercise magnifies the affect by increasing baseline blood pressure through increased heartrate and muscle pump activity. Two anatomical circumstances suggest how the mechanism operates: (1) bone influx and efflux vessels outside bone are contained within fascia bounded compartments, which include skeletal muscle, and (2) efflux vessels (veins) are valved.”
“During the same exercise vascular resistance in bone increases two to fourfold while vasodilation in adjacent muscle increases”<-So blood flow in muscles increase while blood flow in bone decreases. This could in fact increase hydrostatic pressure in bone as hydrostatic pressure is the force exerted by a fluid at rest and vascular resistance implies that there’s more fluid at rest.
“Solitons in arteries propagate to capillary beds where they increase intravascular hydraulic pressure in fluid unable to escape through veins. In any given osteon or Haversian canal capillary filtration is increased driving extravascular fluid over perivascular
tissue and through nearest canaliculi. Pressures generated during exercise above heartbeat baselines can be considerable; interstitial values as high as 570 mmHg”
” IMP is a poor indicator of blood flow in bone the blood pressure changes associated with its increase are significant. (2) Blood flow to limb bones increases during exercise. (3) Vascular resistance in limb bones increases during exercise”
“contraction of the quadriceps muscle causes a 30 mmHg or more rise in femur IMP”
The Key Role of the Blood Supply to Bone.
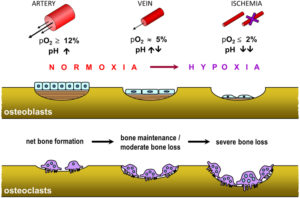
“Blood supplies oxygen, nutrients and regulatory factors to tissues, as well as removing metabolic waste products such as carbon dioxide and acid. Bone receives up to about 10% of cardiac output, and this blood supply permits a much higher degree of cellularity, remodelling and repair than is possible in cartilage, which is avascular. The blood supply to bone is delivered to the endosteal cavity by nutrient arteries, then flows through marrow sinusoids before exiting via numerous small vessels that ramify through the cortex. The marrow cavity affords a range of vascular niches that are thought to regulate the growth and differentiation of hematopoietic and stromal cells, in part via gradients of oxygen tension. The quality of vascular supply to bone tends to decline with age and may be compromised in common pathological settings, including diabetes, anaemias, chronic airway diseases and immobility, as well as by tumours. Reductions in vascular supply are associated with bone loss. This may be due in part to the direct effects of hypoxia, which blocks osteoblast function and bone formation but causes reciprocal increases in osteoclastogenesis and bone resorption. Common regulatory factors such as parathyroid hormone or nitrates, both of which are potent vasodilators, might exert their osteogenic effects on bone via the vasculature. These observations suggest that the bone vasculature will be a fruitful area for future research.”
” impairment of the blood supply is well-known to reduce growth and repair, cause bone loss and, ultimately, necrosis”<-Maybe this could actually be a good thing as hypoxia is often associated with chondrogenesis.
With severe bone loss comes the space for neo-growth plate formation.
“drugs used to treat hypertension[high blood pressure] can increase systemic blood flow”
“High physical activity level has been associated with high bone mass”

“increased venous pressure can promote new bone formation in the periosteum. The data indicated that increased venous pressure will increase blood supply from the capillaries to the bone tissue”
“muscle force alone, if applied at a low rate, such as resistant weight lifting with high intensity, would not be able to generate sufficient strain and fluid pressure in bone. MS with a relatively high rate and a small magnitude, however, can trigger significant fluid pressure in the skeleton.”
“mechanical loading has been shown to reduce sclerostin levels in bone”