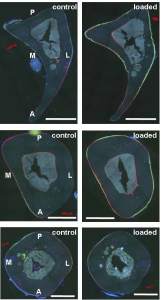
This study shows that the increase in spinal height after bed rest and space flight may be due to an increase in GAG content in the intervertebral disc.
“During spaceflight, it has been shown that intervertebral discs (IVDs) increase in height, causing elongation of the spine up to several centimeters. Astronauts frequently report dull lower back pain that is most likely of discogenic origin and may result from IVD expansion. It is unknown whether disc volume solely increases by water influx, or if the content of glycosaminoglycans also changes in microgravity. Aim of this pilot study was to investigate effects of the spaceflight analog of bedrest on the glycosaminoglycan content of human lumbar IVDs. Five healthy, non-smoking, male human subjects of European descent were immobilized in 6° head-down-tilt bedrest for 21 days. Subjects remained in bed 24 h a day with at least one shoulder on the mattress. Magnetic Resonance Imaging (MRI) scans were taken according to the delayed gadolinium-enhanced magnetic resonance imaging (dGEMRIC) protocol before and after bedrest. The outcome measures were T1 and ΔT1. Scans were performed before and after administration of the contrast agent Gd-DOTA, and differences between T1-values of both scans (ΔT1) were computed. ΔT1 is the longitudinal relaxation time in the tissue and inversely related to the glycosaminoglycan-content. For data analysis, IVDs L1/2 to L4/5 were semi-automatically segmented. Zones were defined and analyzed separately. Results show a highly significant decrease in ΔT1 (p<0.001) after bedrest in all IVDs, and in all areas of the IVDs. The ΔT1-decrease was most prominent in the nucleus pulposus and in L4/5, and was expressed slightly more in the posterior than anterior IVD. Unexpected negative ΔT1-values were found in Pfirrmann-grade 2-discs after bedrest. Significantly lower T1 before contrast agent application was found after bedrest compared to before bedrest. According to the dGEMRIC-literature, the decrease in ΔT1 may be interpreted as an increase in glycosaminoglycans in healthy IVDs during bedrest. This interpretation seems contradictory to previous findings in IVD unloading.”
“Average ΔT1 value of all intervertebral discs was 104.87 ms (sd 7.64 ms) pre-bedrest and -20.20 ms (sd 4.70 ms) post-bedrest.”
“It seems to be well established that increased GAG concentration within the IVD will result in a decrease in ΔT1. A high GAG-concentration causes a small ΔT1 during dGEMRIC-measurements because only small amounts of contrast agent shift into the IVD. A low GAG-concentration in turn leads to a high ΔT1. Increased ΔT1 after an intervention (as compared to before) has been interpreted as degeneration process”<So T1 has nothing to do with the height it has to do with the GAG content. So a decrease in deltaT1 means that GAG content likely increased.