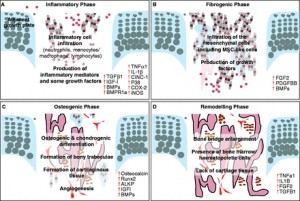
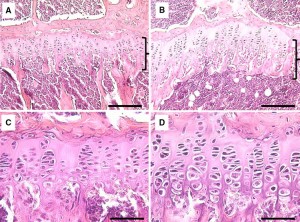
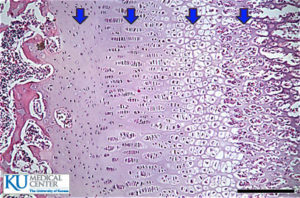
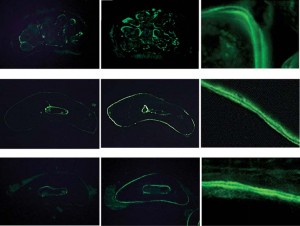
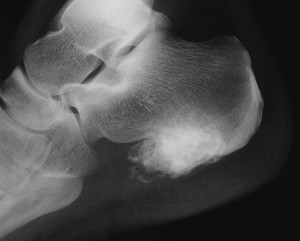
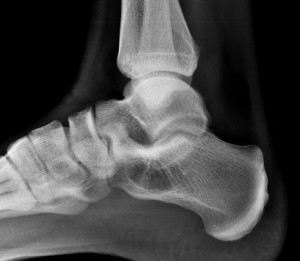
Predicting and Validating the Pathway of Wnt3a-Driven Suppression of Osteoclastogenesis.
“we examined Wnt3a-driven regulation of osteoclast development. Mouse bone marrow-derived cells were incubated with RANKL in the presence and absence of Wnt3a. Using microarray mRNA expression data, we conducted a principal component analysis and predicted transcription factor binding sites (TFBS) that were potentially involved in the responses to RANKL and Wnt3a. The principal component analysis predicted potential Wnt3a responsive regulators that would reverse osteoclast development, and a TFBS prediction algorithm indicated that the AP1 binding site would be linked to Wnt3a-driven suppression. Since c-Fos was upregulated by RANKL and downregulated by Wnt3a in a dose-dependent manner, we examined its role using RNA interference. The partial silencing of c-Fos suppressed RANKL-driven osteoclastogenesis by downregulating NFATc1, a master transcription factor of osteoclast development. Although the involvement of c-Myc was predicted and partial silencing c-Myc slightly reduced the level of TRAP, c-Myc silencing did not alter expression of NFATc1. Collectively, the presented systems-biology approach demonstrates that Wnt3a attenuates RANKL-driven osteoclastogenesis by blocking c-Fos expression and suggests that mechanotransduction of bone alters the development of not only osteoblasts but also osteoclasts through Wnt signaling.”
LSJL upregulates c-Fos. In all likelihood LSJL alters Wnt3a expression but there wasn’t any evidence in the LSJL gene expression study. Fluid flow upregulates Wnt3a and LSJL does involve fluid flow although this was only in osteocytes and we’d want to know the effects on stem cells or chondrocytes for height growth purposes. No evidence that LSJL alters Nfatc1 expression but it likely does and Salubrinal alters Nfatc1 expression. According to a diagram, from that study LSJL would increase Nfactc1 expression but it reduces levels of phosphorylated eif2a.
“Wnt5a activates noncanonical Wnt signaling through a receptor tyrosine kinase-like orphan receptor and stimulates osteoclastogenesis. Wnt10b is required for maintenance of mesenchymal progenitors, and its deficiency leads to loss of bone mass. Wnt14 enhances endochondral ossification and accelerates chondrocyte maturation”<-Wnt14 may alter height. However, Wnt14 does suppress chondrogenic genes and I couldn’t find any studies stating that Wnt14 transgenes or knockout causes overgrowth or undergrowth. Genetic association study of WNT10B polymorphisms with BMD and adiposity parameters in Danish and Belgian males., says that Wnt10b may have an effect on height but more testing needs to be done.
“Mouse bone marrow cells isolated from long bones (femur and tibia) as well as RAW264.7 mouse pre-osteoclast cells [were used in the study]”. If mouse bone marrow cells were used it may have ramifications for how stem cells are affected by stimuli and finding the right stimuli is the key for height growth.
“Administration of RANKL to bone marrow cells significantly increased the number of TRAP-positive multi-nucleated cells{osteoclast cells are trap-positive}. In response to 100 or 200 ng/ml of Wnt3a, the number of TRAP-positive cells was reduced in a dose-dependent manner. The observed suppression of osteoclast development by Wnt3a was associated with a decrease in the phosphorylated form of β-catenin (p-β-catenin) as well as NFATc1 ”
“Wnt3a-induced reduction of the relative mRNA expression levels of the genes (NFATc1, TRAP, OSCAR, MMP9, and cathepsin K) linked to osteoclastogenesis on days 1 and 2 in bone marrow cells”<-Note that none of these levels were lower than control(The cells that were not exposed to RANKL) and the reduction was dose dependent until at least 200ng/ml.
Wnt3a downregulates C-Fos and C-Fos may be an important part in LSJL induced growth.
Wnt3a upregulated Egr1, Notch1, and Tgif1 at greater levels than control so excess levels of Wnt3a may have an effect on stimulating on those genes even without altering cells exposed to RANKL. It downregulated Hmga1, Smad3, Dnmt3a, and Bach1 versus control. Smad3 is involved in TGF-Beta induced chondrogenesis. Dnmt3a promotes DNA methylation.